Understanding Your Microbial Ecosystems
The human microbiome—the vast community of bacteria, fungi, viruses, and other microorganisms living on and in our bodies—has rightfully captured scientific and public attention in recent years. Research reveals that these microbial communities profoundly influence our health, affecting everything from digestion and immunity to mental health and disease susceptibility. Less appreciated but equally important is the home microbiome: the microbial communities inhabiting our living spaces. These two microbiomes don't exist in isolation; they constantly interact, exchanging microbes and influencing each other in ways that affect both household hygiene and human health.
Understanding the connection between human and home microbiomes transforms how we think about cleanliness, hygiene, and health. Rather than viewing our bodies and homes as battlegrounds requiring constant antimicrobial assault, recognising the importance of beneficial microbial communities suggests gentler, more sustainable approaches that cultivate health-promoting bacteria whilst discouraging harmful ones. This ecological perspective aligns perfectly with probiotic cleaning principles.
The Human Microbiome: An Overview
The human body hosts trillions of microorganisms, with bacterial cells roughly equalling human cells in number. These microbes aren't random contamination—they're evolved partners that provide essential services. Intestinal bacteria aid digestion, synthesise vitamins, train immune systems, and prevent pathogenic colonisation. Skin bacteria produce antimicrobial compounds, compete with pathogens for resources and attachment sites, and maintain healthy skin pH.
Different body sites host distinct microbial communities. The gut microbiome, richest in bacterial diversity, contains hundreds of species adapted to the anaerobic, nutrient-rich intestinal environment. Skin microbiomes vary by location—oily facial skin hosts different communities than dry forearms or moist armpits. Oral microbiomes differ between tongue, teeth, and gums. Each community comprises species specifically adapted to local conditions.
Healthy microbiomes resist pathogenic invasion through competitive exclusion, maintaining dense beneficial populations that leave little room or resources for harmful bacteria. This colonisation resistance represents a crucial defence mechanism—one that conventional hygiene practices often undermine by indiscriminately killing beneficial and harmful bacteria alike.
The Home Microbiome: Your House Has a Microbiome Too
Just as our bodies host microbial communities, so do our homes. Every surface—kitchen counters, bathroom fixtures, floors, furniture, door handles—harbours bacterial populations whose composition depends on environmental conditions, surface materials, and the human and animal occupants who continuously seed these communities with microbes from their own microbiomes.
Home microbiomes vary dramatically between households. Homes with pets host different microbial communities than pet-free homes. Houses in different climates support distinct bacteria adapted to local temperature and humidity. Cleaning practices profoundly affect home microbiomes: homes cleaned primarily with probiotic products develop different microbial communities than those cleaned with harsh disinfectants.
Recent research reveals that home microbiomes aren't simply contamination—they affect occupant health. Diverse home microbiomes associate with reduced allergy and asthma risk, particularly in children. Homes with dogs introduce microbial diversity that may protect against immune disorders. Conversely, extremely sterile homes might deprive developing immune systems of the microbial exposure necessary for healthy development.
The Exchange: How Microbiomes Interact
Human and home microbiomes constantly exchange microbes. Every time you touch a surface, you deposit bacteria from your skin microbiome. Every breath releases bacteria from oral and respiratory microbiomes into the air, where they settle on surfaces. Conversely, touching surfaces transfers bacteria to your skin. Consuming food prepared on contaminated surfaces introduces environmental bacteria to your gut.
This bidirectional exchange means your home microbiome significantly influences your personal microbiome and vice versa. Studies show that household members share more similar microbiomes than strangers, reflecting their shared home environment. Couples have more similar skin microbiomes than people living apart. Dogs alter their owners' home and personal microbiomes, introducing outdoor bacterial diversity.
The practical implication is profound: you cannot separate personal hygiene from environmental hygiene. Maintaining a healthy home microbiome supports healthy personal microbiomes. Conversely, excessive antimicrobial product use that damages home microbiomes can indirectly affect personal microbiome health.
Beneficial Bacteria: Partners in Both Environments
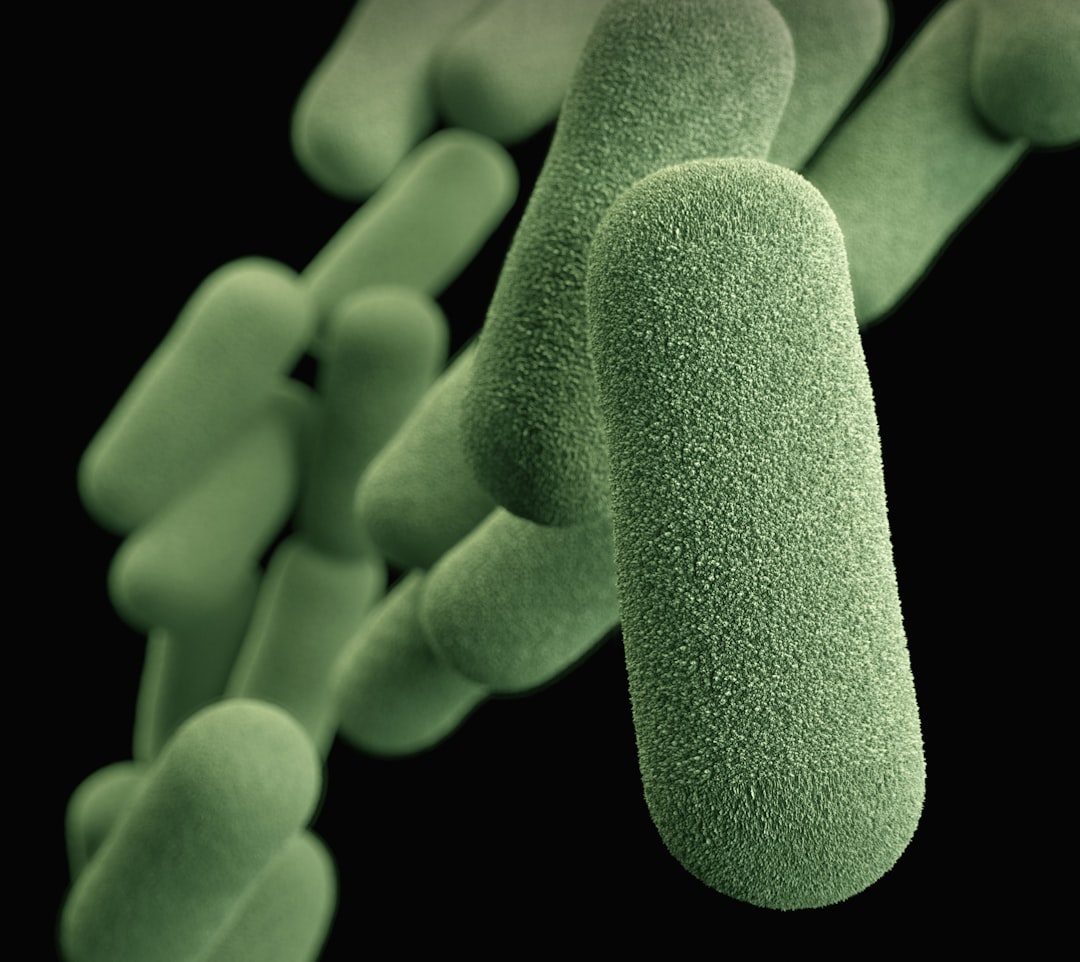
Many beneficial bacterial species colonise both human and home environments. Bacillus species, common soil bacteria, naturally occur on human skin and in intestines whilst also colonising household surfaces, particularly in homes with gardens or outdoor access. Certain Lactobacillus species inhabit both the human gut and fermented foods stored in refrigerators.
These shared beneficial species provide protection in both environments. On skin, they compete with pathogens and produce antimicrobial compounds. On household surfaces, they perform similar competitive and antimicrobial functions. Moving between environments, they seed both locations with beneficial populations.
Probiotic cleaning deliberately enhances beneficial bacterial presence in home environments. By introducing Bacillus and sometimes Lactobacillus species, probiotic products establish populations of bacteria already adapted to human coexistence. These bacteria don't merely tolerate human presence—they evolved alongside humans and often benefit human health through their competitive suppression of pathogens.
Pathogenic Bacteria: Crossing Boundaries
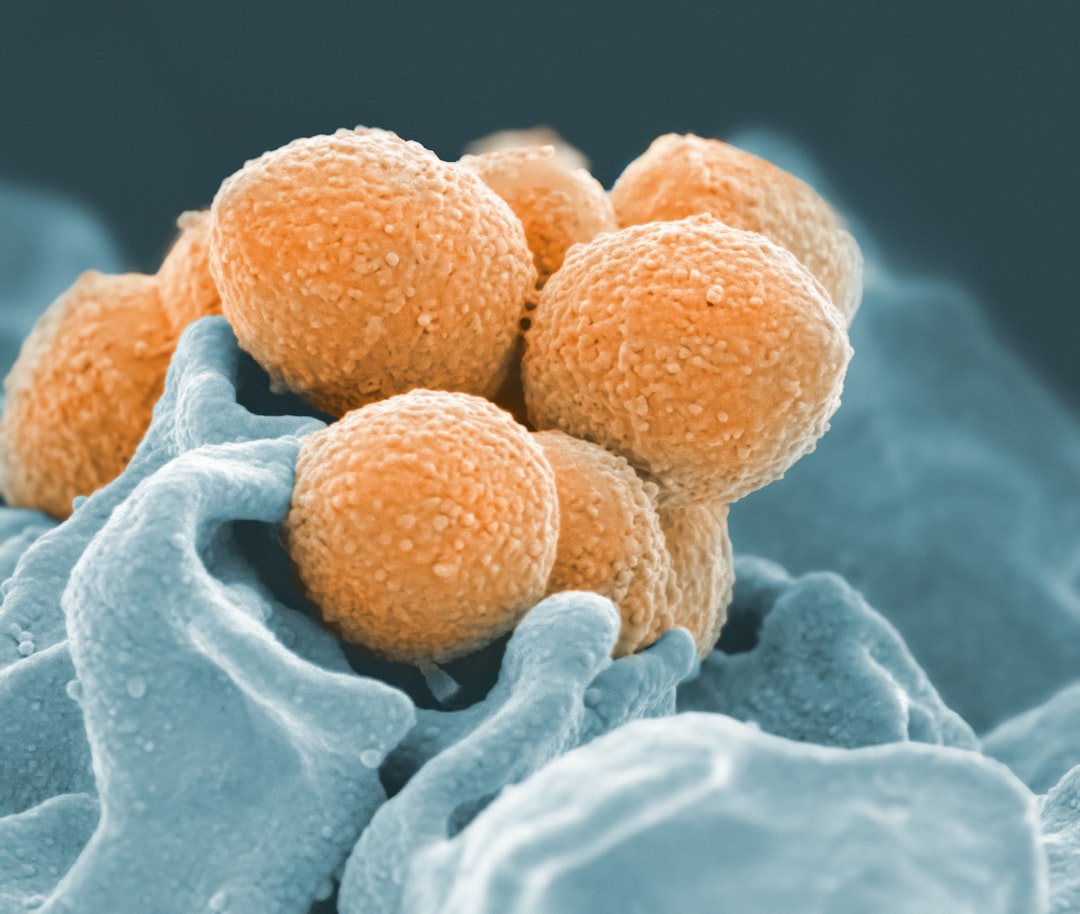
Unfortunately, pathogenic bacteria also cross between human and home environments. Staphylococcus aureus colonises human noses and skin, spreading to household surfaces through contact. From surfaces, it can transfer to other household members or back to the original carrier, potentially causing infections if it enters wounds or reaches susceptible tissues.
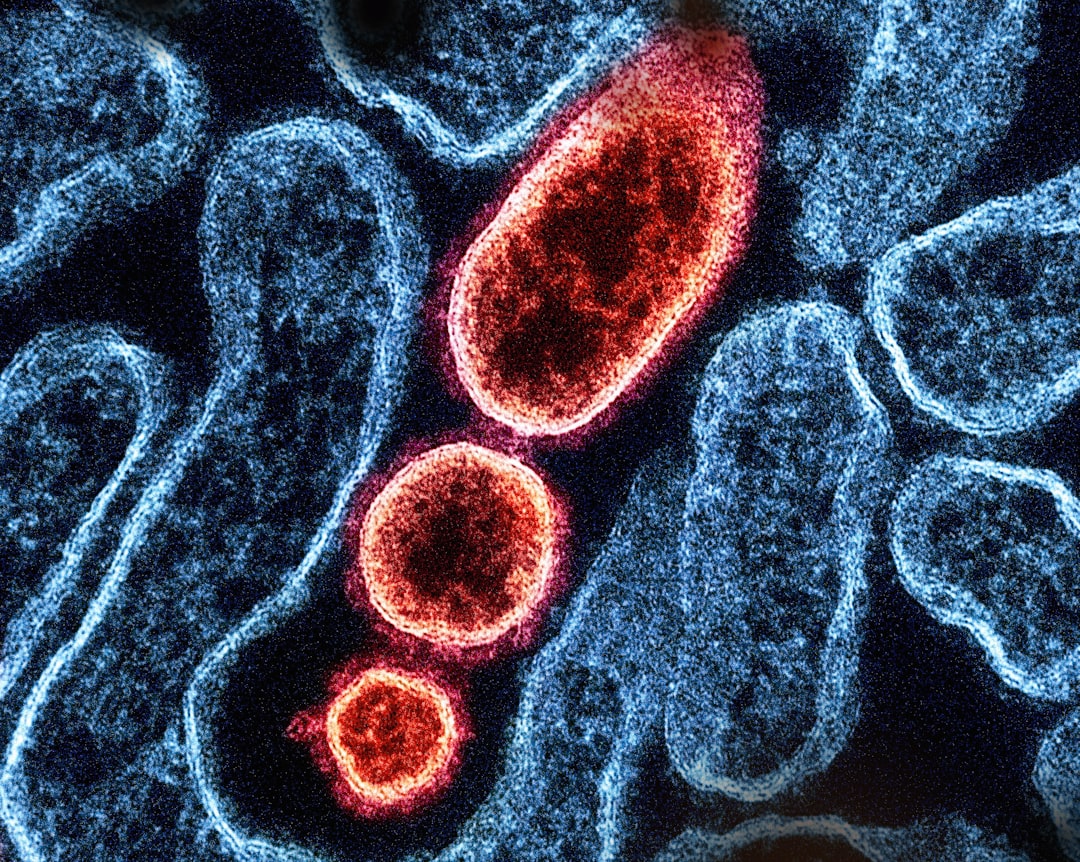
Escherichia coli normally lives harmlessly in intestines but causes illness if pathogenic strains reach food preparation surfaces, contaminating foods that are then consumed. Kitchen environments thus serve as critical transfer points where intestinal bacteria can move from one person to others through environmental contamination.
Breaking these transmission cycles requires understanding the pathogen's journey. Hand hygiene after toilet use prevents intestinal bacteria from reaching surfaces. Proper food handling prevents surface bacteria from contaminating foods. Establishing beneficial bacterial populations on surfaces reduces pathogenic survival and persistence, decreasing transmission risk even when contamination occurs.
The Hygiene Hypothesis and Microbial Exposure
The hygiene hypothesis proposes that reduced microbial exposure during childhood contributes to increased allergy and autoimmune disease rates in developed countries. Whilst controversial in details, the underlying principle finds increasing support: developing immune systems require microbial exposure to mature properly. Overly sterile environments might deprive immune systems of necessary training, leading to dysfunctional responses including allergies and autoimmunity.
This hypothesis doesn't suggest abandoning hygiene—rather, it suggests distinguishing between exposure to beneficial or harmless bacteria versus dangerous pathogens. Children benefit from encountering diverse environmental bacteria from soil, pets, and varied environments. They don't benefit from exposure to enteric pathogens from faecal contamination or respiratory pathogens from sick individuals.
Probiotic cleaning supports beneficial microbial exposure whilst reducing pathogenic risks. It maintains diverse bacterial communities in home environments—providing immune-training exposure—whilst specifically suppressing dangerous pathogens through competitive exclusion. This balanced approach supports immune development without compromising safety.
Antibiotics and Microbiome Disruption
Antibiotic use, whilst sometimes medically necessary, disrupts both personal and home microbiomes. Antibiotics kill susceptible bacteria indiscriminately, eliminating beneficial species alongside pathogens. This disruption creates ecological vacuums that antibiotic-resistant bacteria or opportunistic pathogens rapidly fill.
After antibiotic treatment, patients shed resistant and opportunistic bacteria into their home environments, altering home microbiome composition. These environmental bacteria can recolonise the recovering patient or colonise other household members, spreading resistant strains. This vicious cycle—antibiotics disrupt microbiomes, releasing resistant bacteria that spread through environments—drives antimicrobial resistance in both clinical and community settings.
Probiotic interventions during and after antibiotic treatment may help mitigate this disruption. Consuming probiotic foods or supplements helps maintain intestinal beneficial bacteria despite antibiotic pressure. Using probiotic cleaners maintains beneficial bacteria in home environments, reducing the ecological space available for resistant bacteria or opportunistic pathogens to colonise during the vulnerable post-antibiotic period.
Cleaning Practices and Microbiome Health
Traditional cleaning practices using harsh disinfectants dramatically affect home microbiomes, typically reducing bacterial diversity and selecting for resistant strains. Initially, disinfectants kill most bacteria, creating what appears to be a clean surface. However, this microbial desert rapidly recolonises with whatever bacteria arrive first—often resistant strains or fast-growing opportunists rather than the diverse communities that existed previously.
Repeated disinfection creates selection pressure favouring resistant bacteria. Over time, home microbiomes in heavily disinfected houses shift towards resistant and opportunistic species, potentially including more pathogenic bacteria than homes cleaned with gentler methods. This counterintuitive outcome—more intensive disinfection potentially creating less safe microbial communities—highlights the importance of ecological thinking in hygiene practices.
Probiotic cleaning maintains or increases home microbiome diversity by introducing beneficial bacteria that establish self-sustaining populations. Rather than creating microbial vacuums through killing, it creates beneficial dominance through competition. The resulting diverse, beneficial-dominated communities resist pathogenic colonisation more effectively than the resistant-dominated communities that develop under repeated disinfection.
Specific Home Locations and Microbiome Connections
Kitchens serve as critical connection points between home and human microbiomes, particularly regarding intestinal bacteria. Food preparation involves extensive hand-surface contact, creating numerous opportunities for bacterial transfer. Establishing beneficial bacterial communities on kitchen surfaces reduces pathogenic persistence, decreasing foodborne illness risk.
Bathrooms, particularly toilets and associated surfaces, inevitably host faecal bacteria from human microbiomes. Whilst concerning, most faecal bacteria are harmless residents of healthy intestinal microbiomes. Probiotic bathroom cleaning suppresses genuinely pathogenic enteric bacteria whilst tolerating harmless intestinal species, maintaining bathroom microbiomes that reflect normal human microbial ecology rather than pathogen-dominated communities.
Bedrooms and sleeping areas host bacteria primarily from skin and respiratory microbiomes. Bedding accumulates skin bacteria, creating communities that then recolonise sleeper's skin. Beneficial bacteria in these environments may support healthy skin microbiomes, whilst pathogenic species like Staphylococcus aureus can establish reservoir populations in bedding that repeatedly colonise skin.
Pets and Microbiome Diversity
Pet ownership profoundly affects home microbiomes. Dogs and cats introduce soil bacteria, outdoor environmental bacteria, and their own commensal bacteria into homes. This increased microbial diversity generally proves beneficial, particularly for children, reducing allergy risk and supporting immune development.
However, pets can also introduce pathogens. Dog faeces can carry Campylobacter or Salmonella. Cat scratches introduce Bartonella. Proper pet hygiene—cleaning litter boxes promptly, washing hands after pet contact, treating pets for parasites—reduces pathogenic risks whilst preserving beneficial microbial diversity pet ownership provides.
Building a Healthy Home Microbiome
Cultivating healthy home microbiomes requires balanced approaches. Regular cleaning removes excessive organic matter and reduces overall bacterial loads, preventing overgrowth. Using probiotic cleaners introduces beneficial bacteria that establish protective populations. Maintaining appropriate ventilation and moisture control creates environmental conditions favouring beneficial over pathogenic bacteria.
Allowing appropriate microbial exposure—spending time outdoors, interacting with pets, gardening—introduces beneficial environmental diversity. However, maintaining targeted hygiene in critical areas—hand washing, food preparation surface cleaning, toilet hygiene—prevents dangerous pathogen transmission.
This balanced approach recognises that we cannot and should not eliminate all bacteria from our bodies or homes. Instead, we should cultivate beneficial bacterial communities in both environments, creating ecological stability that naturally suppresses pathogens whilst supporting health. Understanding the connection between human and home microbiomes makes this ecological approach not merely sensible but essential for long-term health and hygiene.